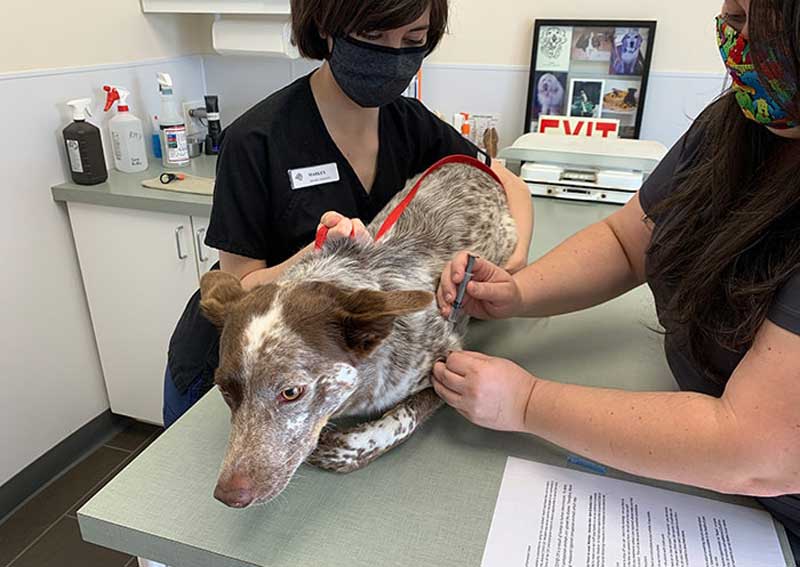
Welcome To Crossroads Veterinary Hospital!
Crossroads Veterinary Hospital is a full-service facility that strives to provide the very best veterinary care to our patients. Our top rated Sherwood veterinarians offer a variety of veterinary services, including:
- Preventive Care & Wellness
- Dentistry
- Advanced Diagnostics
- Surgery
- Pet Allergy & Dermatology
- Urgent Care
- and many more!
We look forward to working with you to provide the best care possible for your family members.
Call us at (503) 625-4404 or book an appointment online today!
Canine Respiratory Disease on the Rise: What You Need to Know
An unknown, possibly severe form of canine cough is on the rise; owners can help ensure their pet’s health by recognizing symptoms early. Learn about symptoms, preventive measures, and what to do if your pet shows signs of this mysterious respiratory disease. Learn More »Pet First Aid Awareness
Being prepared with basic first aid supplies in the event of an emergency is part of being a responsible pet parent. There are a few items to consider having on hand in your own pet first aid kit. We’ve put together a list of these recommended items. Remember, the use of these items should only be used temporarily until your pet can be seen and examined by a veterinarian.
Learn More »Our Clients Love Us

They are ready and able to take care of our dogs even in those emergency times when most vets are closed
Drannan Tidwell

Nice Vets!
michael eagle

4.7
Rating on
Google Reviews!